Do you suffer from urticaria (hives)?
General information
Urticaria, commonly known as hives, is a skin condition marked by itchy, swollen patches of various sizes. Typically, hives appear suddenly and resolve within a few hours. These temporary lesions do not leave any lasting marks, indicating that the skin is not damaged.
When the swelling extends to deeper layers of the skin, it is called angioedema. Angioedema develops in up to half of those with hives. Both conditions can manifest simultaneously.
Urticaria is quite prevalent, affecting one in five people at some point. It is often non-allergic, so it is not unusual for an allergist to advise against allergy testing.
Sometimes, it represents an actual allergic reaction caused by a food, a medication, an insect sting, or another sensitizing agent. Your allergist will indicate if this is your case. If you suddenly develop hives or angioedema along with other symptoms such as trouble breathing, tightness in the throat, nausea or vomiting, cramping abdominal pain, or passing out, you should seek medical attention as soon as possible.
Classification of urticaria
1. Acute urticaria
Allergic urticaria

Urticaria
Other than certain reactions to medication, the allergic cause of urticaria is easily recognized by the afflicted individual. In general, urticaria follows less than 30 minutes after ingestion or contact with the sensitizing agent (food, insect sting, latex, etc.). Skin tests can be very useful in confirming the diagnosis of allergy.
Pseudo-Allergic urticaria
Several substances labelled as "non-specific histamine liberators" can provoke urticaria. Among these agents, the classics are codeine, morphine, several antibiotics, radio-contrast products used in radiology, and the curates (general anesthesia). Numerous foods (strawberries, fermented products, alcohol, honey, etc.) in addition to aspirin (ASA) and other anti-inflammatories can provoke a "pseudo-allergic" urticaria quite rapidly in predisposed subjects. Unfortunately, in all of these cases, allergy tests are unreliable.
2. Chronic urticaria
When hives last more than 6 weeks, this is called chronic urticaria or chronic spontaneous urticaria. This form of urticaria is mostly NOT allergic and can sometimes be challenging to treat.
Although chronic hives can last for years, in about half of cases, the symptoms typically resolve on their own in under 6 months. Most cases of chronic hives do not require an extensive workup since a specific cause is usually not found.
Sometimes, urticaria is associated with an auto-immune disease, thyroid disease, cancer, or an infection (viral infection, parasites, helicobacter pylori, for example). Common viral infections may be self-limited, but the cause may need to be treated in some cases.
3. Inducible or physical urticaria
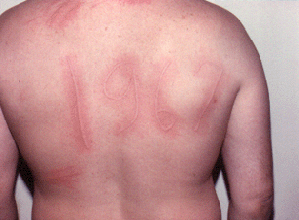
Dermographism
Diverse physical stimuli (heat, exercise, the sun, cold, pressure and vibration) may provoke urticaria. This kind of urticaria is called "physical" and often occurs rapidly (several minutes) after a physical stimulus, except in certain cases of pressure urticaria, where symptoms may be delayed. Dermographism is one form of physical urticaria.
Late-onset pressure urticaria (belt, bras, hands of a manual labourer, etc.) is often chronic, difficult to treat, and characterized by warm rather than itchy lesions.
Treatment of urticaria
Treatment of urticaria may be through pharmacological or non-pharmacological means, often depending on the cause.
Non-Pharmacological
- Avoid factors that evoke the physical urticarias, such as excessive heat, the sun, tight clothing or irritants, etc.
- Avoid vasodilatory factors which may potentialize urticaria, such as alcohol, nicotinic acid, anti-inflammatories, several anti-hypertensive medications and diverse food "irritants" (such as acidic foods, spices, fermented foods and charcuterie).
- Treat, if possible, any disease that may cause the urticaria (secondary urticaria or angioedema).
Pharmacological
- Symptomatic urticaria is treated with antihistamines, usually newer non-sedating agents with prolonged half-lives (cetirizine, loratadine, desloratadine, fexofenadine).
- In the case of treatment failure with conventional medication, the allergist may prescribe biological medications such as omalizumab, or other immune modulating agents.
__________________________
Ana Copaescu, MD, PhD (text)
John Weisnagel, MD (photos)
Updated 03/2025
 The Association of Allergists and Immunologists of Québec
The Association of Allergists and Immunologists of Québec